Entry
Reader's guide
Entries A-Z
Subject index
Contraception Methods
Contraception allows women to choose the number and spacing of their children. Female sterilization and intrauterine devices (IUDs) account for almost 40 percent in less developed countries, and combined oral contraceptive pills (COC), IUDs, and condoms for the same proportion in more developed countries. Contraception remains one of the most cost-effective public health measures to reduce rates of maternal and infant mortality.
In 2008, modern contraception prevented about 188 million unintended pregnancies, 1.2 million newborn deaths, and 230,000 pregnancy related deaths. An unmet need for family planning of an estimated 215 million women of reproductive age who want to avoid or postpone childbearing still exists because they are not using effective contraceptive methods. There are several reasons for this, including lack of knowledge about the risk of becoming pregnant, fear of side effects of contraceptives, influence from partners and community leaders, religious beliefs, and lack of access or finances to use family planning services. A large number of unintended pregnancies occur due to lack of knowledge and myths regarding contraception and the failure or discontinuation of use of short-term hormonal contraception. Effectiveness of a contraceptive method depends on compliance and correct use of that method. It is thus essential that proper information and counseling on contraception choices for both women and men should be advocated. Health practitioners should be able to discuss all eligible contraceptive methods locally available. Essential topics should include effectiveness, risks and side effects, and advantages and disadvantages.
Choosing a Method
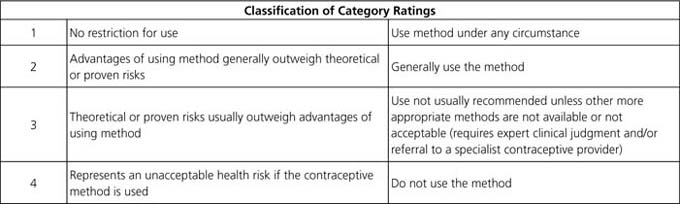
The World Health Organization (WHO) produced guidelines to aid in contraceptive choice. The WHO Medical Eligibility Criteria for Contraceptive Use (WHO MEC) provides evidence-based recommendations to help the healthcare provider to safely select the most appropriate method of contraception. A WHO also provides information on contraception effectiveness to assists in decision making. Table I provides classifications of the four categories used.
Women must realize that popular methods, such as COCs and barrier contraception, that rely on daily or coital administration have “typical” use failure rates (user and method failures) that are higher than the “perfect” use rates (method failures). Their effectiveness is dependent on compliance and correct use. This has resulted in the promotion of “long-acting reversible contraception” (LARC). A LARC is a method that requires administration less than once per cycle or month. These methods include copper IUDs, levonorgestrel-intrauterine systems (LNGIUS), progestogen-only injectable contraceptives (POIC), progestogen-only subdermal implants, and combined hormonal vaginal rings. LARC methods combine reversibility with high effectiveness.
Table 1: World Health Organization Contraceptive Use Classification
Natural Methods
Natural family planning methods are practiced in most countries and include fertility-based methods (FAM) and withdrawal. These methods are safe, have no side effects, are inexpensive to practice, and may be easily discontinued.
Disadvantages include meticulous recordkeeping of fertility cycles, involve intensive training, and are dependent on a partner's willingness to abstain from intercourse during the fertile period. Other factors, such as irregular menstrual cycles, medicine that may affect body temperature or cervical mucus, women who are breastfeeding or ill, as well as cervical surgery may influence effectiveness.
...
- Activism in Theory and Practice
- Animal Rights
- Arab Feminism
- Bat Shalom—Jerusalem Women's Action Center
- Chicana Feminism
- Children's Rights
- Codepink
- Critical Race Feminism
- Domestic Violence Centers
- Eagle Forum
- EMILY's List
- Environmental Activism, Grassroots
- Family Research Council
- Feminism on College Campuses
- Feminist Majority Foundation
- Feminists for Life
- Focus on the Family
- Gay and Lesbian Advocacy
- General Union of Palestinian Women
- Global Feminism
- Granny Peace Brigade
- Independent Women's Forum
- Indigenous Women's Rights: Bolivia
- Iranian Feminism
- Islamic Revolution in Iran
- MADRE
- Million Mom March
- Mothers Against Choice
- Mothers Against Drunk Driving
- NARAL
- National Organization for Women
- National Women's Political Caucus
- Organization of Women's Freedom in Iraq
- Panchita's House: Domestic Workers Rights in Lima, Peru
- Peace Movement
- Rape Crisis Centers
- Revolutionary Association of the Women of Afghanistan
- Signal Biographies: Brady, Sarah
- Signal Biographies: Ebadi, Shirin
- Signal Biographies: Ensler, Eve
- Signal Biographies: Ghozlan, Engy Ayman
- Signal Biographies: LaDuke, Winona
- Signal Biographies: Linton, Simi
- Signal Biographies: Mairs, Nancy
- Signal Biographies: Mankiller, Wilma
- Signal Biographies: Michelman, Kate
- Signal Biographies: Zajovic, Stanislava Stasa
- Social Justice: Activism
- Take Back the Night
- Third Wave
- Tibetan Women's Association
- Transnational Feminist Networks
- Vagina Monologues, The
- White Supremacy
- Womanism
- Women in Black
- Women Involved in Farm Economics
- Women's International League for Peace and Freedom
- Arts
- Australian Aboriginal Artistse
- Bollywood
- Classical Music, Women in
- Country and Western Music, Women in
- Dance, Women in
- Dinner Party, The (Judy Chicago)
- Film Actors, Female
- Film Directors, Female
- Film Production, Women in
- Guerrilla Girls
- Hip Hop
- National Museum of Women in the Arts
- Novelists, Female
- Photography, Women in
- Poets, Female
- Representation of Women
- Signal Biographies: Chicago, Judy
- Signal Biographies: Coppola, Sofia
- Signal Biographies: Duffy, Carol Ann
- Signal Biographies: Holzer, Jenny
- Signal Biographies: Kngwarreye, Emily
- Signal Biographies: Leibovitz, Annie
- Signal Biographies: Lessing, Doris
- Signal Biographies: Morrison, Toni
- Signal Biographies: Oates, Joyce Carol
- Signal Biographies: Parton, Dolly
- Signal Biographies: Showalter, Elaine
- Signal Biographies: Te Kanawa, Dame Kiri
- Signal Biographies: Walker, Alice
- Signal Biographies: Walker, Kara
- Signal Biographies: Zaimont, Judith Lang
- Studio Arts, Women in
- Sweet Honey in the Rock
- Visual Arts, Women in
- Women Make Movies
- Business, Commerce, and Economics
- 9to5
- Association for Women's Rights in Development
- CEOs, Female
- Child Labor
- Cosmetics Industry
- Cowgirls
- Crafting Industry
- Diet Industry
- Direct Sales
- Domestic Workers
- Economics, Women in
- Entrepreneurs
- Equal Pay
- Fair Trade
- Fashion Industry
- Financial Independence of Women
- Glass Ceiling
- Grameen Bank of Bangladesh
- International Monetary Fund
- International Women's Day
- Management
- Management Styles, Gender Theories
- Maquiladoras
- Mentoring
- Microcredit
- Migrant Workers
- Nannies
- Nontraditional Careers, U.S.
- Parental Leave
- Part-Time Work
- Partner Rights
- Philanthropists, Female
- Poverty
- Poverty, Feminization of
- Sewa in India
- Sex Workers
- Sexual Harassment
- Signal Biographies: Ledbetter, Lilly
- Signal Biographies: Mehta, Renu
- Signal Biographies: Nooyi, Indra
- Signal Biographies: Stewart, Martha
- Sweatshops
- Trafficking, Women and Children
- Unions
- United Nations Development Fund for Women
- Unpaid Labor
- Wedding Industry
- Women's Cooperatives
- Women's Funding Network
- Women's Thrift Cooperatives
- Work/Life Balance
- Countries
- Africa
- Algeria
- Angola
- Benin
- Botswana
- Burkina Faso
- Burundi
- Côte D'Ivoire
- Cameroon
- Cape Verde
- Central African Republic
- Chad
- Comoros
- Congo
- Congo, Democratic Republic
- Djibouti
- Egypt
- Equatorial Guinea
- Eritrea
- Ethiopia
- Gabon
- Gambia
- Ghana
- Guinea
- Guinea-Bissau
- Kenya
- Lesotho
- Liberia
- Madagascar
- Malawi
- Mali
- Mauritania
- Mauritius
- Morocco
- Mozambique
- Namibia
- Niger
- Nigeria
- Rwanda
- São Tomé and Principe
- Senegal
- Sierra Leone
- Somalia
- South Africa
- Sudan
- Swaziland
- Tanzania
- Togo
- Tunisia
- Uganda
- Zambia
- Zimbabwe
- Americas
- Antigua and Barbuda
- Argentina
- Bahamas
- Barbados
- Belize
- Bolivia
- Brazil
- Canada
- Chile
- Colombia
- Costa Rica
- Cuba
- Dominica
- Dominican Republic
- Ecuador
- El Salvador
- Grenada
- Guatemala
- Guyana
- Haiti
- Honduras
- Jamaica
- Mexico
- Nicaragua
- Panama
- Paraguay
- Peru
- Saint Kitts and Nevis
- Saint Lucia
- Saint Vincent and the Grenadines
- Suriname
- Trinidad and Tobago
- United States
- Uruguay
- Venezuela
- Asia
- Afghanistan
- Azerbaijan
- Bahrain
- Bangladesh
- Bhutan
- Brunei Darussalam
- Cambodia
- China
- East Timor
- Georgia
- India
- Indonesia
- Iran
- Iraq
- Israel
- Japan
- Jordan
- Kazakhstan
- Kuwait
- Kyrgyzstan
- Laos
- Lebanon
- Malaysia
- Maldives
- Moldova
- Mongolia
- Myanmar
- Nepal
- Oman
- Pakistan
- Palestine
- Philippines
- Qatar
- Russia
- Saudi Arabia
- Seychelles
- Singapore
- Sri Lanka
- Syria
- Tajikistan
- Thailand
- Turkey
- Turkmenistan
- Ukraine
- United Arab Emirates
- Uzbekistan
- Vietnam
- Yemen
- Europe
- Albania
- Andorra
- Armenia
- Austria
- Belarus
- Belgium
- Bosnia and Herzegovina
- Bulgaria
- Croatia
- Cyprus
- Czech Republic
- Denmark
- Estonia
- Finland
- France
- Germany
- Greece
- Hungary
- Iceland
- Ireland
- Italy
- Latvia
- Liechtenstein
- Lithuania
- Luxembourg
- Macedonia (FYROM)
- Malta
- Monaco
- Netherlands
- Norway
- Poland
- Portugal
- Romania
- San Marino
- Serbia and Montenegro
- Slovakia
- Slovenia
- Spain
- Sweden
- Switzerland
- United Kingdom
- Pacific
- Africa
- Education
- Adjunct and Contingent Faculty
- American Association of University Women
- Attainment, College Degree
- Attainment, Elementary School Completion
- Attainment, Graduate Degree
- Attainment, High School Completion
- Campaign for Female Education
- College and University Faculty
- Community Colleges
- Educational Administrators, College and University
- Educational Administrators, Elementary and High School
- Educational Attainment, Effect of Unpaid Labor on
- Educational Opportunities/Access
- Elementary Educators
- Family and Consumer Sciences
- Fields of Study
- Financial Aid
- Forum for African Women Educationalists
- Girl-Friendly Schools
- Global Campaign for Education
- Hate Speech and Bias on College Campuses
- High School Teachers
- Home Schooling
- National Women's Studies Association
- No Child Left Behind
- Professional Education, Trade/Vocational Schools
- School Fee Abolition Initiative
- Signal Biographies: al-Faiz, Norah
- Signal Biographies: Jackson, Shirley Ann
- Signal Biographies: Nascimento, Adir Casaro
- Signal Biographies: Tamang, Stella
- Single Sex Education
- Title IX
- Vocational and Trade School Faculty
- Women's Colleges
- Women's Resource Centers
- Women's Studies
- Environment
- Birth Defects: Environmental Factors
- Cancer: Environmental Factors
- Climate Change as a Women's Issue
- Drought
- Ecofeminism
- Environmental Justice
- Famine
- Green Belt Movement
- International Conference on Population and Development
- Locavorism/Slow Food Movement
- Love Canal
- Navdanya
- Overpopulation
- Rachel's Network
- Signal Biographies: Brockovich, Erin
- Signal Biographies: Gibbs, Lois
- Signal Biographies: Maathai, Wangari
- Signal Biographies: Plumwood, Val
- Signal Biographies: Shiva, Vandana
- Signal Biographies: Waters, Alice
- Toxic Waste as a Women's Issue
- Vegetarian Feminism
- Water as a Women's Issue
- Women's Environment and Development Organization
- Government/Law and Justice
- Affirmative Action/Equal Opportunity
- AMBER Alerts
- Attorneys, Female
- Convention on the Rights of the Child
- Convention to End Discrimination Against Women
- Council of Women World Leaders
- Crime Victims, Female
- Drug Trade
- Equal Rights Amendment
- Feminist Jurisprudence
- Gender Quotas in Government
- Girl Gangs
- Guns and Gun Use
- Hate Crimes
- Heads of State, Female
- Honor Killings
- Honor Suicides
- International Action Network on Small Arms
- Judges, Women as
- Law Enforcement, Women in
- League of Women Voters
- Lilly Ledbetter Act
- Megan's Law
- Nongovernmental Organizations
- Parental Leave Act
- Perpetrators, Female
- Political Ideologies
- Prison Administration
- Prison Guards, Female (U.S.)
- Prisoners, Female (U.S.)
- Rape, Legal Definitions of
- Rape, Prosecution Rates
- Representation of Women in Government: International
- Representation of Women in Government: U.S.
- Roe v. Wade
- Self-Defense, Armed
- Self-Defense, Unarmed
- Sex Offenders, Female
- Sex Offenders, Male
- Signal Biographies: Albright, Madeleine
- Signal Biographies: Bachelet, Michelle
- Signal Biographies: Bhutto, Benazir
- Signal Biographies: Bruntland, Gro Harlem
- Signal Biographies: Clinton, Hillary Rodham
- Signal Biographies: Gandhi, Sonia
- Signal Biographies: Ginsberg, Ruth Bader
- Signal Biographies: Kirchner, Cristina Fernández de
- Signal Biographies: Merkel, Angela
- Signal Biographies: O'Connor, Sandra Day
- Signal Biographies: Obama, Michelle
- Signal Biographies: Palin, Sarah
- Signal Biographies: Pelosi, Nancy
- Signal Biographies: Queen Noor
- Signal Biographies: Rice, Condoleezza
- Signal Biographies: Robinson, Mary
- Signal Biographies: Sarkozy, Carla Bruni
- Signal Biographies: SigurÐardóttir, Jóhanna
- Signal Biographies: Sirleaf, Ellen Johnson
- Signal Biographies: Thatcher, Margaret
- Social Justice Theory
- United Nations Conferences on Women
- United Nations Conventions
- Violence Against Women Act
- Voting Rights
- White House Council on Women and Girls
- Health: Mental and Physical
- Abortion Laws: International
- Abortion Methods
- Abortion, Access to
- Addiction and Substance Abuse
- Anxiety Disorders
- Bariatric Surgery
- Birth Defects
- Body Image
- Botox
- Breast Cancer
- Breast Reduction Surgery
- Caesarean Section, Rates of
- Chastity Pledges
- Childbirth Methods, Cross-Cultural
- Childbirth, Home Versus Hospital
- Childbirth, Medication in
- Contraception Methods
- Cosmetic Surgery
- Crisis Pregnancy Centers
- Depression
- Diabetes
- Diagnostic and Statistical Manual of Mental Disorders
- Diagnostic and Statistical Manual of Mental Disorders, Critiques of
- Disability: Definitions
- Doulas
- Dysthymia in Minority Population
- Eating Disorders
- Fecundity
- Female Genital Surgery, Geographical Distribution
- Female Genital Surgery, Terminology and Critiques of
- Female Genital Surgery, Types of
- Fertility
- Freedom of Choice Act
- Freedom of Conscience Legislation
- Gardasil
- Gender Dysphoria
- Gender Reassignment Surgery
- Global “Gag Rule”
- Health Insurance Issues
- Heart Disease
- HIV/AIDS: Africa
- HIV/AIDS: Asia
- HIV/AIDS: Europe
- HIV/AIDS: North America
- HIV/AIDS: Oceania
- HIV/AIDS: South America
- Hysterectomies
- Infant Mortality
- Infanticide
- Infertility, Incidence
- Infertility, Treatments
- Life Expectancy, International Comparisons of
- Maternal Mortality
- Medical Research, Gender Issues
- Menopause: Medical Aspects
- Menopause: Social Aspects
- Menstruation
- Mental Health Treatment, Access to
- Mental Health Treatment, Bias in
- Mental Illness, Incidence Rates
- Midwifery
- Nurses
- Nutrition
- Nutrition in Pregnancy
- Obsessive Compulsive Disorder
- Physicians Assistants, Female
- Physicians, Female
- Physicians, Specialties
- Plan B
- Planned Parenthood
- Post-Abortion Trauma Syndrome
- Postmenstrual Dysphoric Disorder
- Postpartum Depression
- Postpartum Psychosis
- Pregnancy
- Premenstrual Syndrome
- Prenatal Care
- Psychotropic Medications
- Puberty
- Rape and HIV
- Rape Trauma Syndrome
- Rape, Cross-Culturally Defined
- Rape, Incidence of
- Rates of Psychological Disorders by Gender
- Reproductive Cancers
- Reproductive Health Issues
- Reproductive Rights
- Revirginization
- RU-486
- Self-Mutilation
- Sex Education, Abstinence-Only
- Sex Education, Comprehensive
- Sex Education, Cross-Culturally Compared
- Sexually Transmitted Infections
- Signal Biographies: Bowers, Marci
- Signal Biographies: Dirie, Waris
- Signal Biographies: Elders, Joycelyn
- Signal Biographies: Gomperts, Rebecca
- Signal Biographies: McCorvey, Norma
- Signal Biographies: Solomon, Suniti
- Signal Biographies: Suleman, Nadia
- Signal Biographies: Yates, Andrea
- Snowflake Babies
- Sterilization
- Sterilization, Involuntary
- Suicide and Race
- Suicide Methods
- Suicide Rates
- Women's Health Clinics
- World Health Organization
- Media/Popular Culture
- Action Heroes, Female
- Advertising, Aimed at Women
- Advertising, Female Professionals in
- Advertising, Portrayal of Women in
- American Girl Dolls
- Anime
- Barbie Dolls
- Beauty Pageants
- Beauty Pageants (Babies/Young Children)
- Blogs and the Blogosphere
- Body Art
- Bratz Dolls
- Cartoonists, Female
- Celebrity Women
- Censorship
- Cougars
- Disc Jockeys
- Dora the Explorer
- Feminist Publishing
- Hello Kitty
- Journalists, Broadcast Media
- Journalists, Print Media
- Manga
- Media Chief Executive Offcers, Female
- Ms. Magazine
- Our Bodies, Ourselves
- Pink, Advertising and
- Pornography Produced by Women
- Pornography, Portrayal of Women in
- Pornography/Erotica
- Reality Television
- Roller Derby
- Romance Novels
- Signal Biographies: Amanpour, Christiane
- Signal Biographies: Banks, Tyra
- Signal Biographies: Couric, Katie
- Signal Biographies: DeGeneres, Ellen
- Signal Biographies: Ehrenreich, Barbara
- Signal Biographies: Goody, Jade
- Signal Biographies: Hefner, Christie
- Signal Biographies: Huffngton, Arianna
- Signal Biographies: Maddow, Rachel
- Signal Biographies: Madonna
- Signal Biographies: Paglia, Camille
- Signal Biographies: Queen Latifah
- Signal Biographies: Steinem, Gloria
- Signal Biographies: Thomas, Helen
- Signal Biographies: vanden Heuvel, Katrina
- Signal Biographies: Walters, Barbara
- Signal Biographies: Winfrey, Oprah
- Slasher Movies
- Soap Operas, Cross-Culturally Considered
- Sports Illustrated Swimsuit Edition
- Toys, Gender-Stereotypic
- Women's Cable Networks
- Women's Magazines
- Religion
- African American Muslims
- Anglican Communion
- Black Churches
- Buddhism
- Candomblé
- Catholics for Choice
- Chabad Movement
- Chinese Religions
- Christian Identity
- Christianity
- Clergy Abuse/Pedophilia
- Contraception: Religious Approaches
- Creation Care Movement (Evangelical)
- Da Vinci Code, The
- Evangelical Protestantism
- Feminist Theology
- Fundamentalist Christianity
- Fundamentalist Church of Jesus Christ of Latter-Day Saints
- Hindu Female Gurus and Living Saints
- Hinduism
- Homosexuality, Religious Attitudes
- Indigenous Religions, Global
- Islam
- Islam in America
- Islamic Feminism
- Judaism
- Ku Klux Klan
- Kumari, Living Goddess in Nepal
- Lesbian/Gay Clergy
- Machismo/Marianismo
- Mary Magdalene
- Metropolitan Community Church
- Ministry: Protestant
- Mormon Church/Church of Jesus Christ of Latter-day Saints
- Mujerista Theology
- Native American Religion
- New Age Religion
- Nuns: Buddhist
- Nuns: Roman Catholic
- Operation Rescue
- Orthodox Churches
- Orthodox Judaism
- Polygamy, Cross-Culturally Considered
- Priesthood: Episcopalian/Anglican
- Priesthood: Roman Catholic
- Pro-Life Movement
- Progressive Muslims (U.S.)
- Purity Balls
- Rabbis, Female
- Religious Fundamentalisms, Cross-Culturally Considered
- Revolve
- Roman Catholic Church
- Santería
- Secularity Law, France
- Sharià Law
- Signal Biographies: Johnson, Sonia
- Signal Biographies: Pagels, Elaine
- Signal Biographies: Schori, Katharine Jefferts
- Signal Biographies: Starhawk
- Signal Biographies: Wadud, Amina
- Signal Biographies: Winkett, Canon Lucy
- Sikhism
- Southern Baptist Convention
- Stem Cell Research: Religious Arguments for and Against
- Suttee
- Taliban
- Veil
- Virgin Mary
- Virgin of Guadalupe
- Voodoo
- Wahabism
- Wicca/Goddess Spirituality
- Witchcraft: Worldwide
- Womanist Theology
- Women's Ordination Conference
- Yoga
- Science and Technology
- Astronauts, Female
- Astronomy, Women in
- Biology, Women in
- Chatrooms
- Chemistry, Women in
- Computer Games
- Computer Science, Women in
- Earth Science, Women in
- Engineering, Women in
- Internet
- Internet Dating
- Mathematics, Women in
- Multiverses, Gender Stereotypes in
- Pedophilia Online
- Physics, Women in
- Science Education for Girls
- Sexting
- Signal Biographies: Barré-Sinoussi, FranÇoise
- Signal Biographies: Grandin, Temple
- Signal Biographies: Ride, Sally
- Signal Biographies: Shoemaker, Carolyn
- Signal Biographies: Villa-Komaroff, Lydia
- Stem Coalition
- Veterinarians, Female
- Sports and Recreation
- Auto Racing: Formula One
- Auto Racing: NASCAR
- Basketball: College
- Beach Volleyball/Volleyball
- Boxing
- Coaches of Women's Teams
- Coaches, Female
- Cowboy Action Shooting
- Dykes on Bikes
- Exercise Science
- Figure Skating
- Fitness
- Golf
- Gymnastics
- Horse Racing, Women in
- Hunting
- Little League
- Olympics: Summer
- Olympics: Winter
- Pilates
- Rodeo
- Running/Marathons
- Shooting Sports, Women in
- Signal Biographies: Ali, Laila
- Signal Biographies: Kim, Yu-Na
- Signal Biographies: Patrick, Danica
- Signal Biographies: Rhode, Kim
- Signal Biographies: Sörenstam, Annika
- Signal Biographies: Torres, Dara
- Signal Biographies: Visser, Lesley
- Signal Biographies: Williams, Venus and Serena
- Soccer, Children's
- Soccer, Professional
- Sports Announcers, Female
- Sports Offcials, Female
- Steroid Use
- Swimming
- Team Owners, Female
- Tennis
- Track and Field
- Weightlifting
- Women's National Basketball Association
- Xtreme Sports
- Sexualities
- Africa
- Asia
- Bisexuality
- Civil Unions
- Coming Out
- Drag Kings
- Europe
- Gender, Defined
- Heterosexism
- Heterosexuality
- Homophobia
- Human Rights Campaign
- Intersex
- Lesbian Adoption
- Lesbians
- LGBTQ
- North America
- Oceania
- Parents, Families and Friends of Lesbians and Gays
- Queer Theory
- Same-Sex Marriage
- Sex Education in the Home
- Sex, Defined
- Sexual Orientation
- Sexual Orientation and Race
- Sexual Orientation, Theories of Causation
- Sexual Orientation–Based Legal Discrimination: Outside United States
- Sexual Orientation–Based Legal Discrimination: United States
- Sexual Orientation–Based Social Discrimination: Outside United States
- Sexual Orientation–Based Social Discrimination: United States
- Sexual Orientation–Based Violence: Outside United States
- Sexual Orientation–Based Violence: United States
- Signal Biographies: Chase, Cheryl
- Signal Biographies: Feinberg, Leslie
- Signal Biographies: Flannery, Sarah
- Signal Biographies: Shepard, Judy
- Signal Biographies: Vincent, Norah
- Transgender
- Two-Spirit
- War and Conflict
- Abu Ghraib
- Combat, Women in
- Community Defense/Resistance
- Conflict Zones
- Guerrilla Fighters, Female
- Land Mines
- Lesbians in the Military
- Military Leadership, Women in
- Military Stationed in Muslim Countries
- Military, Women in
- Post-Traumatic Stress Disorder in Female Military
- Prisoners of War, Female
- Prostitution in Combat Zones
- Rape in Conflict Zones
- Signal Biographies: Cornum, Rhonda
- Signal Biographies: Drif, Zohra
- Signal Biographies: Duckworth, Tammy
- Signal Biographies: England, Lynndie
- Signal Biographies: Karpinski, Janis
- Suicide Bombers, Female
- Terrorists, Female
- Wars of National Liberation, Women in
- Women's Lives
- Adoption
- Aging, Attitudes Toward
- Antifeminism
- Beauty Standards, Cross-Cultural
- Child Abuse Perpetrators
- Child Abuse Victims
- Childcare
- Childlessness as Choice
- Dating Violence
- Diet and Weight Control
- Divorce
- Domestic Violence
- Elder Abuse
- Family, Career, and Community Leaders of America
- Fatherlessness
- Femininity, Social Construction of
- Feminism
- Foster Mothers
- Gender Roles: Cross-Cultural
- Girl Scouts
- Girls, Inc.
- Grandmothers
- Helicopter Parents
- Homemakers and Social Security
- Homemaking
- Household Decision-Making
- Mail-Order Brides
- Marriage
- Marriages, Arranged
- Masculinity, Social Construction of
- Mistresses
- Mothers in Prison
- Property Rights
- Quinceañeras
- Rural Women
- Security Moms
- Single Mothers
- Soccer Moms
- Stay-at-Home Mothers
- Stereotypes of Women
- Teen Pregnancy
- Welfare
- Widows
- Working Mothers
- Loading...
Get a 30 day FREE TRIAL
-
Watch videos from a variety of sources bringing classroom topics to life
-
Read modern, diverse business cases
-
Explore hundreds of books and reference titles

Sage Recommends
We found other relevant content for you on other Sage platforms.

Have you created a personal profile? Login or create a profile so that you can save clips, playlists and searches