Entry
Entries A-Z
Subject index
Chronic Disease Management
Disease management means taking actions to ensure the best possible level of health and functioning for the individual and the least amount of disruption of daily life. Implicit in the concept of chronic disease is the idea that no cure for the given illness is available and the condition must be managed to reduce its impact on the patient, family, and society.
Management strategies comprise an individual's means to keep the disease and its effects under control (Clark, 1998; Karoly & Kanfer, 1982). These strategies may be effective or ineffective and may be consistent with clinicians' recommendations or not. Some people left to themselves will derive ways to achieve disease control that physicians or health educators would applaud (e.g., a susceptible asthma patient removing environmental precipitants to symptoms from the living quarters). Many do not (e.g., the person with asthma overusing bronchodilators in an effort to reduce symptoms). Effective disease control requires a strong partnership between patient, family, and clinician and adequate support from the health system and community to the individual who must manage the condition from day to day. Disease management is undertaken in full recognition that actions will not eliminate the disease but reduce its impact, for example, prolong life, enhance functioning, and in some instances reduce costs.
Similar themes run across definitions of chronic disease management by the patient (Creer, Levstek, & Reynolds, 1998; Karoly & Kanfer, 1982). First, 90% to 98% of day-to-day management is carried out by the patient. Second, recommended regimens involve a changing and complex set of behaviors and are not allor-none phenomena (Glasgow & Eakin, 1998). Third, the context (setting and conditions) in which one manages influences the strategies utilized (Creer et al., 1998). Fourth, effective management by the patient requires a shift from well-established, habitual or automatic but ineffective responses to problems toward systematic long-term effective control. Longterm success entails attention to internal and external factors and use of cognitive processes to increase effectiveness (Karoly & Kanfer, 1982). Fifth, unless psychopathology or severe physical limitation is present, individuals can learn to improve their management of disease (Clark et al., 1986).
Description
Until chronic diseases became the primary concern of developed countries, both professionals and patients, used to dealing with acute conditions, believed and behaved as if the manager of illness was the physician (or other relevant clinician) (Clark et al., 1995; Wagner, Austin, & Von Korff, 1996b). In recent years, however, it has become accepted that patients are the managers of their conditions. Of course, patients cannot do the job alone, as many aspects of disease control lie outside their ability or authority. Figure 1 illustrates the circles of influence on the individual trying to keep the effects of illness to a minimum (Clark et al., 1995).
Figure 1 Concentric Circles of Influence
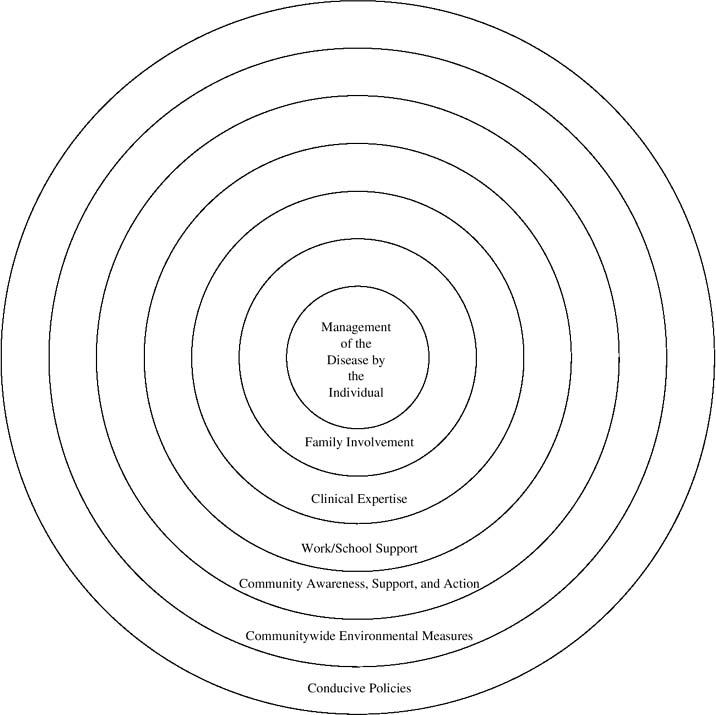
The most influential is the family (Wasilewski et al., 1988), as members are in closest proximity to the patient and often, particularly in the case of a child, actually perform management tasks on behalf of the patient. Clinical expertise is also central to effective disease management (Clark et al., 2000). Most if not all chronic diseases require partnership between the physician and patient, with the clinician providing the best possible therapeutic regimen as well as the counseling and education that enables the patient to carry through the clinical recommendations (Clark et al., 1995). The actions of the individual physician (or nurse or related clinical professional) are to a great extent influenced by the procedures of the organizations that provide and/or handle payments for clinical services. The availability, structure, policies, and resources of health provider organizations have a significant impact on how enabled or not a patient is in efforts to manage chronic disease. Other people in the social environment of the person with a chronic condition (work, school, and home) help or hinder effective management, as do individuals and organizations in the wider community. Communitywide policies and resources also have an effect.
...
- Loading...
Get a 30 day FREE TRIAL
-
Watch videos from a variety of sources bringing classroom topics to life
-
Read modern, diverse business cases
-
Explore hundreds of books and reference titles

Sage Recommends
We found other relevant content for you on other Sage platforms.

Have you created a personal profile? Login or create a profile so that you can save clips, playlists and searches